http://www.lifeextension.com/Magazine/2018/7/Fish-Oil-Reduces-Inflammatory-Fires/Page-01?utm_source=facebook&utm_medium=social&utm_campaign=organicpost
By Clyde Pepper
Many ill effects of aging are caused by low-grade, chronic inflammation.
These slow-burning internal fires damage tissues and underlie many cancers, vascular disorders, and dementias.
Inflammation is partially regulated through the eicosanoid pathway.
Age, poor diet, and other factors tip the balance of this pathway from anti-inflammatory to pro-inflammatory.
Omega-3-rich fish oil rebalances the eicosanoid pathway and safely helps reduce inflammation.
What is the Eicosanoid Pathway?
The eicosanoid pathway is a signaling pattern that regulates inflammation when needed.
The eicosanoid pathway helps turn on inflammation when it’s needed and turn it off once it has done its job. This is accomplished through signaling molecules called eicosanoids.
There are two types of these signaling molecules—one that is pro-inflammatory, and one that is anti-inflammatory.
The pro-inflammatory signaling molecules are produced from omega-6 polyunsaturated fatty acids, whereas the anti-inflammatory molecules are mostly produced from omega-3 polyunsaturated fatty acids.1-5
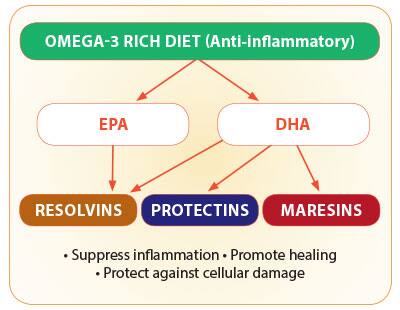
Omega-3 also produces three additional classes of signaling molecules—called resolvins, protectins, and maresins. These go beyond suppressing inflammation by also promoting healing and actively protecting against cellular damage.3-8
The ratio of omega-6 to omega-3 is a major factor in determining whether the eicosanoid pathway will produce predominantly pro-inflammatory or anti-inflammatory signals.
Our typical Western diet contains far more omega-6 than omega-3 fats—an imbalance that pushes our eicosanoid pathway towards pro-inflammatory signaling, resulting in chronic inflammation.2
Fish oil improves the ratio of omega-6 to omega-3 thus reducing the incidence of age-associated inflammatory disorders—including cardiovascular, autoimmune, metabolic, and neurodegenerative diseases.
Inflammation-driven disease takes us down the road to premature disability and death. Reversing that inflammation with EPA- and DHA-rich fish oil represents a means of slowing certain aging processes.
In the next sections, we’ll review the evidence showing how fish oil supplements can have a beneficial impact on inflammatory-related conditions.
Fish Oil Reduces Chronic Inflammation
- Inflammation triggers a cascade of destructive changes in cell and tissue function that leave us vulnerable to diabetes, cardiovascular disease, neurodegeneration, and even losses of bone and joint integrity.
- New studies show that we can control the balance of the eicosanoid pathway, tipping it back towards a low-inflammation, pro-resolution state, by supplementing with fish oil rich in the omega-3 fatty acids EPA and DHA.
- Animal and human studies now demonstrate the usefulness of fish oil supplements rich in EPA and DHA in mitigating the impact of diabetes, cardiovascular disease, neurodegenerative conditions, and skeletal health.
- Fish oil can be considered a fundamental anti-aging supplement because of its potent regulation of the eicosanoid pathway.
Cardiovascular Disease
Cardiovascular disease—which includes heart attacks, hypertension, strokes, atrial fibrillation, and heart failure—remains one of the leading killers worldwide.9
Inflammatory changes contribute to every point in the cascade of events that lead to cardiovascular catastrophe.
This includes promoting the development of atherosclerotic plaques and platelet clumping in arteries, as well as disrupting the electrical network of the heart itself.
Reducing the burden of inflammation is an important way to attack cardiovascular diseases before they become problematic. Fish oil/omega-3 supplementation is emerging as an important way to accomplish this task.
Human studies show that populations that consume large amounts of oily fish have reduced incidence of and deaths from cardiovascular disorders. This is due in part to fish oil’s ability to help lower triglycerides and reduce evidence of atherosclerosis.10,11 Omega-3 fish oil supplements have also been shown to improve endothelial function and stabilize arterial plaques (making them less likely to rupture and obstruct an artery).10
EPA and DHA omega-3s produce profound shifts from the pro-inflammatory eicosanoids to protective, anti-inflammatory, vessel-dilating eicosanoids.12
There has long been interest in the ability of omega-3 supplementation to reduce the risk of atrial fibrillation, which is a cardiac rhythm disturbance that affects up to a third of people with hypertension.13 Atrial fibrillation can increase the risk of strokes and death, and is associated with inflammatory changes in the heart’s electrical system.13
Ultimately—and most importantly—fish oil consumption has been shown to reduce coronary heart disease-related deaths.11
Neurodegenerative Disorders
Alzheimer’s disease is the most prevalent neurodegenerative disorder. Inflammation plays a major role in its development.14
Omega-3s from fish oil are involved in both the reduction and resolution of inflammation through their impacts on the eicosanoid pathway—making them promising for the prevention of this debilitating disease.
Growing evidence indicates that, while DHA and EPA work together, they also have distinct individual influences on brain health.14 For example, EPA has been shown to improve symptoms of mood disorders (depression, anxiety), while DHA has a role in maintaining normal brain structures.14 Omega-3s cross the normally impermeable blood-brain barrier, making them available directly to brain cells.15
Studies of blood cells from Alzheimer’s disease patients show that supplementing with DHA and EPA for six months causes significant alterations in 19 genes involved in inflammation, neurodegeneration, and resolution of inflammation. This suggests that these beneficial fatty acids are regulating gene expression, which is a powerful epigenetic effect.16
Many of those changes result in increased production of three signaling molecules derived from omega-3s: resolvins, protectins, and maresins.17 As we learned earlier, these compounds have the dual benefit of resolving inflammation while also helping repair damaged tissue.
One way these omega-3-derived signaling factors afford protections is by increasing white blood cells’ appetite for consuming beta-amyloid, the toxic protein found in the brains of those with neurodegenerative diseases, while also reducing inflammation in the brain.8
Levels of these signaling molecules are reduced in people with Alzheimer’s disease and in those with minimal cognitive impairment (which commonly precedes Alzheimer’s).8,17,18
Omega-3 supplementation has been shown to beneficially support levels of these specialized molecules.17
One study showed that cognitive function in supplemented Alzheimer’s patients was closely associated with higher levels of resolvins, protectins, and maresins. Another showed benefit only in those with mild cognitive impairment, a grim reminder that early intervention is critical.8
An encouraging study in 2016 showed that supplementing with fish oil directly impacts brain size and structure in people with mild cognitive impairment.19 While placebo recipients in this study had decreased volume of gray matter in brain areas associated with Alzheimer’s disease, those taking the fish oil supplement (combined with aerobic exercise and cognitive stimulation) had unchanged, and in some cases increased volume of gray matter, the region of the brain involved in everything from memory and speech to emotions and decision-making.19
Those findings help explain results of an earlier study, in which Alzheimer’s patients who supplemented with omega-3 had less decline in activities of daily living compared with placebo recipients. And when lipoic acid was added to the supplement, subjects showed even less decline in cognitive function.20
The typical Western diet today contains a vast excess of omega-6 fats (largely derived from poultry products and certain vegetable oils).41,42
The optimum ratio of omega-6 to omega-3 fats in the diet is roughly 4 to 1, though some proponents claim the ratio should be two omega-6s for each one omega-3. Shockingly, those who follow unhealthy modern Western diets often consume these fats in ratios as high as 25 (omega-6) to only 1 (omega-3).2,41
Diabetes
Type II diabetes is a ballooning epidemic that follows directly in the path of obesity and inflammation-driven insulin resistance. Fish oil’s ability to combat inflammation naturally protects against diabetes and its effects.
Animal research shows that fish oil supplementation improves metabolic factors associated with type II diabetes, including improving glucose tolerance (less insulin resistance) and decreased blood and liver lipid levels.21
Human studies have also demonstrated the benefits of omega-3s in diabetic patients. In one study, 30 obese type II diabetics took omega-3 supplements while following a protein-enriched diet with low glycemic-index carbohydrates. After 24 weeks, their hemoglobin A1c levels (a marker of chronic blood sugar elevation) diminished 11.1%, their waist circumference was reduced by 1.3 inches, and they experienced a significant reduction in C-reactive protein (CRP), the blood marker of inflammation.22
Fish oil/omega-3 supplements also protect us against the inflammation-related effects of diabetes.
In patients with type II diabetes, taking 4,000 mg/day of fish oil significantly reduced blood triglycerides and improved kidney function.23 In an animal study, giving diabetic rats fish oil improved diabetes-associated cognitive deficit, suppressed inflammatory changes, and protected brain cells against destruction.23,24
Another major effect of diabetes is an increase in cardiovascular disease. There’s now strong evidence that diets high in omega-3 fish oil can reduce this deadly risk in diabetics by reducing artery-clogging platelet clumping and dangerous lipid elevations.25 Studies also show that diabetics who consume higher amounts of fish oil/omega-3s have lower blood pressure and are up to 19% less likely to die from cardiovascular disease.25,26
Bone Health
Osteoporosis arises from an imbalance between the production of new bone and breakdown of older bone tissue.
The eicosanoid pathway can generate pro-inflammatory molecules created from certain omega-6 fatty acids, leading to inflammatory signals that can contribute to osteoporosis by promoting the activity of cells that break down bone (osteoclasts), while suppressing activity of those that produce new bone (osteoblasts).27-30
Omega-3 supplementation can help counteract this harmful effect, shifting the balance back towards healthier bones. This has been seen in animal studies, which have repeatedly shown that omega-3 supplementation reduces inflammation and protects against bone loss by reducing activity of osteoclasts. This tips the balance toward new bone formation by osteoblasts, and helps to prevent bone fractures.27,31-33
A human study showed that omega-3 supplementation—combined with regular exercise—can reduce inflammatory changes and augment bone mineral density in postmenopausal women, the largest group at risk for osteoporosis.34
Joint Health

Osteoarthritis is the most common cause of joint pain and disability in aging adults.35 The condition involves destruction of joint cartilage and remodeling of the bone just below cartilage—both of which are driven by chronic inflammation.36
Not surprisingly then, adults with higher omega-6 to omega-3 ratios have greater pain, functional limitations, and psycho-social distress compared to those with lower ratios.37
Studies in dogs, which notoriously suffer from osteoarthritis, show that fish oil omega-3 supplementation significantly improves weight-bearing ability and lowers the need for other anti-inflammatory drugs.38,39
A human study from Germany demonstrated that the combination of omega-3 (EPA plus DHA) and glucosamine sulfate reduced morning stiffness and pain in the hips and knees more effectively than glucosamine sulfate alone.40
Summary
Chronic, low-grade inflammation is linked to age-related conditions as varied as type II diabetes, cardiovascular disease risk, cognitive decline, aching joints, and osteoporosis.
We can help control our eicosanoid pathway functions by supplementing with omega-3 fish oil.
The EPA and DHA found in fish oil shifts the eicosanoid pathway into producing anti-inflammatory signals that reduce inflammation. These omega-3s have also been shown to promote the production of recently discovered resolvins, protectins, and maresins, compounds that have the dual benefit of resolving inflammation while also helping repair damaged tissue.
Human and laboratory studies point to an important role of fish oil supplementation in preventing many inflammation-driven, age-associated disorders, including diabetes, cardiovascular disease, neurodegeneration, and even bone and joint disorders.
If you have any questions on the scientific content of this article, please call a Life Extension® Wellness Specialist at 1-866-864-3027.
References
- Mori TA. Marine OMEGA-3 fatty acids in the prevention of cardiovascular disease. Fitoterapia. 2017;123:51-8.
- Wall R, Ross RP, Fitzgerald GF, et al. Fatty acids from fish: the anti-inflammatory potential of long-chain omega-3 fatty acids. Nutr Rev. 2010;68(5):280-9.
- Calder PC. Marine omega-3 fatty acids and inflammatory processes: Effects, mechanisms and clinical relevance. Biochim Biophys Acta. 2015;1851(4):469-84.
- Calder PC. Omega-3 fatty acids and inflammatory processes: from molecules to man. Biochem Soc Trans. 2017;45(5):1105-15.
- Maskrey BH, Megson IL, Rossi AG, et al. Emerging importance of omega-3 fatty acids in the innate immune response: molecular mechanisms and lipidomic strategies for their analysis. Mol Nutr Food Res. 2013;57(8):1390-400.
- Martinez-Fernandez L, Laiglesia LM, Huerta AE, et al. Omega-3 fatty acids and adipose tissue function in obesity and metabolic syndrome. Prostaglandins Other Lipid Mediat. 2015;121(Pt A):24-41.
- Lorente-Cebrian S, Costa AG, Navas-Carretero S, et al. An update on the role of omega-3 fatty acids on inflammatory and degenerative diseases. J Physiol Biochem. 2015;71(2):341-9.
- Fiala M, Terrando N, Dalli J. Specialized Pro-Resolving Mediators from Omega-3 Fatty Acids Improve Amyloid-beta Phagocytosis and Regulate Inflammation in Patients with Minor Cognitive Impairment. J Alzheimers Dis. 2015;48(2):293-301.
- Lambert C, Cubedo J, Padro T, et al. Phytosterols and Omega 3 Supplementation Exert Novel Regulatory Effects on Metabolic and Inflammatory Pathways: A Proteomic Study. Nutrients. 2017;9(6).
- Burke MF, Burke FM, Soffer DE. Review of Cardiometabolic Effects of Prescription Omega-3 Fatty Acids. Curr Atheroscler Rep. 2017;19(12):60.
- Watanabe Y, Tatsuno I. Omega-3 polyunsaturated fatty acids for cardiovascular diseases: present, past and future. Expert Rev Clin Pharmacol. 2017;10(8):865-73.
- Schunck WH, Konkel A, Fischer R, et al. Therapeutic potential of omega-3 fatty acid-derived epoxyeicosanoids in cardiovascular and inflammatory diseases. Pharmacol Ther. 2017.
- Colussi G, Catena C, Fagotto V, et al. Atrial fibrillation and its complications in arterial hypertension: the potential preventive role of omega-3 polyunsaturated fatty acids. Crit Rev Food Sci Nutr. 2018:0.
- Devassy JG, Leng S, Gabbs M, et al. Omega-3 Polyunsaturated Fatty Acids and Oxylipins in Neuroinflammation and Management of Alzheimer Disease. Adv Nutr. 2016;7(5):905-16.
- Freund Levi Y, Vedin I, Cederholm T, et al. Transfer of omega-3 fatty acids across the blood-brain barrier after dietary supplementation with a docosahexaenoic acid-rich omega-3 fatty acid preparation in patients with Alzheimer’s disease: the OmegAD study. J Intern Med. 2014;275(4):428-36.
- Vedin I, Cederholm T, Freund-Levi Y, et al. Effects of DHA-rich n-3 fatty acid supplementation on gene expression in blood mononuclear leukocytes: the OmegAD study. PLoS One. 2012;7(4):e35425.
- Wang X, Hjorth E, Vedin I, et al. Effects of n-3 FA supplementation on the release of proresolving lipid mediators by blood mononuclear cells: the OmegAD study. J Lipid Res. 2015;56(3):674-81.
- Liu-Seifert H, Siemers E, Price K, et al. Cognitive Impairment Precedes and Predicts Functional Impairment in Mild Alzheimer’s Disease. J Alzheimers Dis. 2015;47(1):205-14.
- Kobe T, Witte AV, Schnelle A, et al. Combined omega-3 fatty acids, aerobic exercise and cognitive stimulation prevents decline in gray matter volume of the frontal, parietal and cingulate cortex in patients with mild cognitive impairment. Neuroimage. 2016;131:226-38.
- Shinto L, Quinn J, Montine T, et al. A randomized placebo-controlled pilot trial of omega-3 fatty acids and alpha lipoic acid in Alzheimer’s disease. J Alzheimers Dis. 2014;38(1):111-20.
- Jelinek D, Castillo JJ, Arora SL, et al. A high-fat diet supplemented with fish oil improves metabolic features associated with type 2 diabetes. Nutrition. 2013;29(9):1159-65.
- Moosheer SM, Waldschutz W, Itariu BK, et al. A protein-enriched low glycemic index diet with omega-3 polyunsaturated fatty acid supplementation exerts beneficial effects on metabolic control in type 2 diabetes. Prim Care Diabetes. 2014;8(4):308-14.
- Wong CY, Yiu KH, Li SW, et al. Fish-oil supplement has neutral effects on vascular and metabolic function but improves renal function in patients with Type 2 diabetes mellitus. Diabet Med. 2010;27(1):54-60.
- Jia D, Heng LJ, Yang RH, et al. Fish oil improves learning impairments of diabetic rats by blocking PI3K/AKT/nuclear factor-kappaB-mediated inflammatory pathways. Neuroscience. 2014;258:228-37.
- McEwen B, Morel-Kopp MC, Tofler G, et al. Effect of omega-3 fish oil on cardiovascular risk in diabetes. Diabetes Educ. 2010;36(4):565-84.
- Rudkowska I. Fish oils for cardiovascular disease: Impact on diabetes. Maturitas. 2010;67(1):25
- Tarlton JF, Wilkins LJ, Toscano MJ, et al. Reduced bone breakage and increased bone strength in free range laying hens fed omega-3 polyunsaturated fatty acid supplemented diets. Bone. 2013;52(2):578-86.
- Takeda H, Kikuchi T, Soboku K, et al. Effect of IL-15 and natural killer cells on osteoclasts and osteoblasts in a mouse coculture. Inflammation. 2014;37(3):657-69.
- Chabbi-Achengli Y, Launay JM, Maroteaux L, et al. Serotonin 2B receptor (5-HT2B R) signals through prostacyclin and PPAR-ss/delta in osteoblasts. PLoS One. 2013;8(9):e75783.
- Lutter AH, Hempel U, Anderer U, et al. Biphasic influence of PGE2 on the resorption activity of osteoclast-like cells derived from human peripheral blood monocytes and mouse RAW264.7 cells. Prostaglandins Leukot Essent Fatty Acids. 2016;111:1-7.
- Rahman MM, Bhattacharya A, Banu J, et al. Endogenous n-3 fatty acids protect ovariectomy induced bone loss by attenuating osteoclastogenesis. J Cell Mol Med. 2009;13(8b):1833-44.
- Fernandes G, Bhattacharya A, Rahman M, et al. Effects of n-3 fatty acids on autoimmunity and osteoporosis. Front Biosci. 2008;13:4015-20.
- Wauquier F, Barquissau V, Leotoing L, et al. Borage and fish oils lifelong supplementation decreases inflammation and improves bone health in a murine model of senile osteoporosis. Bone. 2012;50(2):553-61.
- Tartibian B, Hajizadeh Maleki B, Kanaley J, et al. Long-term aerobic exercise and omega-3 supplementation modulate osteoporosis through inflammatory mechanisms in post-menopausal women: a randomized, repeated measures study. Nutr Metab (Lond). 2011;8:71.
- Lopez HL. Nutritional interventions to prevent and treat osteoarthritis. Part I: focus on fatty acids and macronutrients. Pm r. 2012;4(5 Suppl):S145-54.
- Jerosch J. Effects of Glucosamine and Chondroitin Sulfate on Cartilage Metabolism in OA: Outlook on Other Nutrient Partners Especially Omega-3 Fatty Acids. Int J Rheumatol. 2011;2011:969012.
- Sibille KT, King C, Garrett TJ, et al. Omega-6: Omega-3 PUFA Ratio, Pain, Functioning, and Distress in Adults With Knee Pain. Clin J Pain. 2018;34(2):182-9.
- Fritsch DA, Allen TA, Dodd CE, et al. A multicenter study of the effect of dietary supplementation with fish oil omega-3 fatty acids on carprofen dosage in dogs with osteoarthritis. J Am Vet Med Assoc. 2010;236(5):535-9.
- Roush JK, Cross AR, Renberg WC, et al. Evaluation of the effects of dietary supplementation with fish oil omega-3 fatty acids on weight bearing in dogs with osteoarthritis. J Am Vet Med Assoc. 2010;236(1):67-73.
- Gruenwald J, Petzold E, Busch R, et al. Effect of glucosamine sulfate with or without omega-3 fatty acids in patients with osteoarthritis. Adv Ther. 2009;26(9):858-71.
- Caramia G. The essential fatty acids omega-6 and omega-3: from their discovery to their use in therapy. Minerva Pediatr. 2008;60(2):219-33.
- Galland L. Diet and inflammation. Nutr Clin Pract. 2010;25(6): 634-40.
